In ELISA tests, serum and plasma are the most widely used sample types. Differences in sample type, sample preprocessing, and the selection of blood collection tubes can directly affect the accuracy, stability, and repeatability of the assay results. This article focuses on the key differences between serum and plasma and describes the principles for selecting appropriate blood collection tubes.
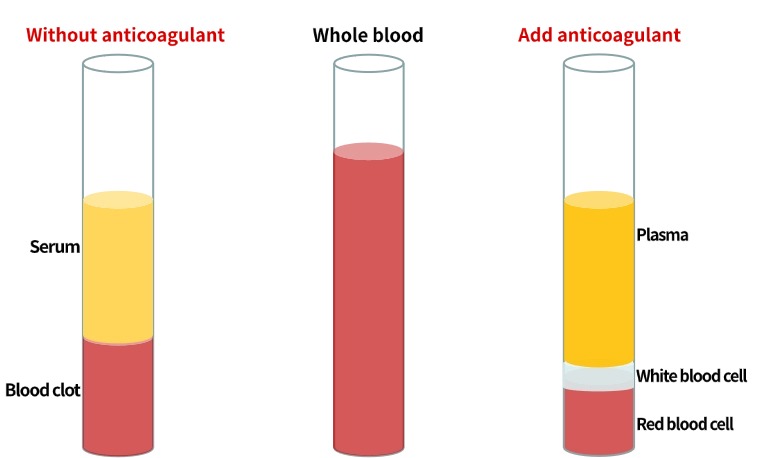
Serum is the pale yellow transparent liquid obtained by removing fibrinogen from the plasma after blood coagulation.
Collection and processing of serum: Use a vacuum blood collection needle to collect fresh blood and add it to a sterile test tube; let it stand at room temperature for 1 hour or overnight at 2-8℃, then centrifuge at 2-8℃, 1000×g for 20 minutes, and take the supernatant for testing.
Plasma is an important component of blood, presenting as a pale yellow liquid (due to the presence of bilirubin).
Collection and processing of plasma: Use a vacuum blood collection needle to collect fresh blood and add it to a sterile test tube; add an anticoagulant at a ratio of 1:9 (the recommended anticoagulant is EDTA-Na2), and separate the plasma within 30 minutes or directly collect it using an anticoagulant tube; After blood collection, place the sample in a centrifuge at 2-8℃, at 1000×g for 15 minutes, and take the supernatant for testing.
Storage of serum/plasma: If collected serum or plasma requires multiple tests, it is recommended to aliquot and freeze them for future use to avoid repeated freeze-thaw cycles.
4℃: Can be stored for one week; -20℃: Can be stored for one month; -80℃: Can be stored for three months.
The commonly used types of blood collection tubes in ELISA tests mainly include the red tube without additives, the yellow tube with a coagulant, the purple tube with EDTA salt, the green tube with heparin, the blue tube with citrate sodium, and the black tube for blood sedimentation.
Red tube: Does not contain any additives. Suitable for routine biochemical serum tests.
Yellow tube: Coagulation-promoting tube, containing a coagulant and inert separation gel. After centrifugation, the separation gel separates the serum and blood cells completely. After collection, it needs to be inverted and mixed 8 times. Suitable for emergency serum biochemical tests.
Purple tube: Tube with EDTA salt for anticoagulation. After collection, it needs to be inverted and mixed 8 times or shaken to mix. Generally suitable for routine blood tests, such as blood routine, blood type, and glycosylated hemoglobin.
Green tube: Also called heparin tube. Heparin directly has an anticoagulant effect and can prolong the clotting time of the specimen. Generally suitable for routine biochemical and emergency plasma tests.
Blue tube: Citrate sodium tube. The anticoagulation ratio (i.e., blood: anticoagulant) is strictly 1:9. After collection, it needs to be inverted and mixed 8 times immediately. Suitable for coagulation function (PT, APTT, fibrinogen, etc.) tests.
Black tube: Blood sedimentation tube. Generally used for coagulation mechanism tests. Anticoagulation ratio is 1:4. After collection, it needs to be inverted and mixed 8 times.
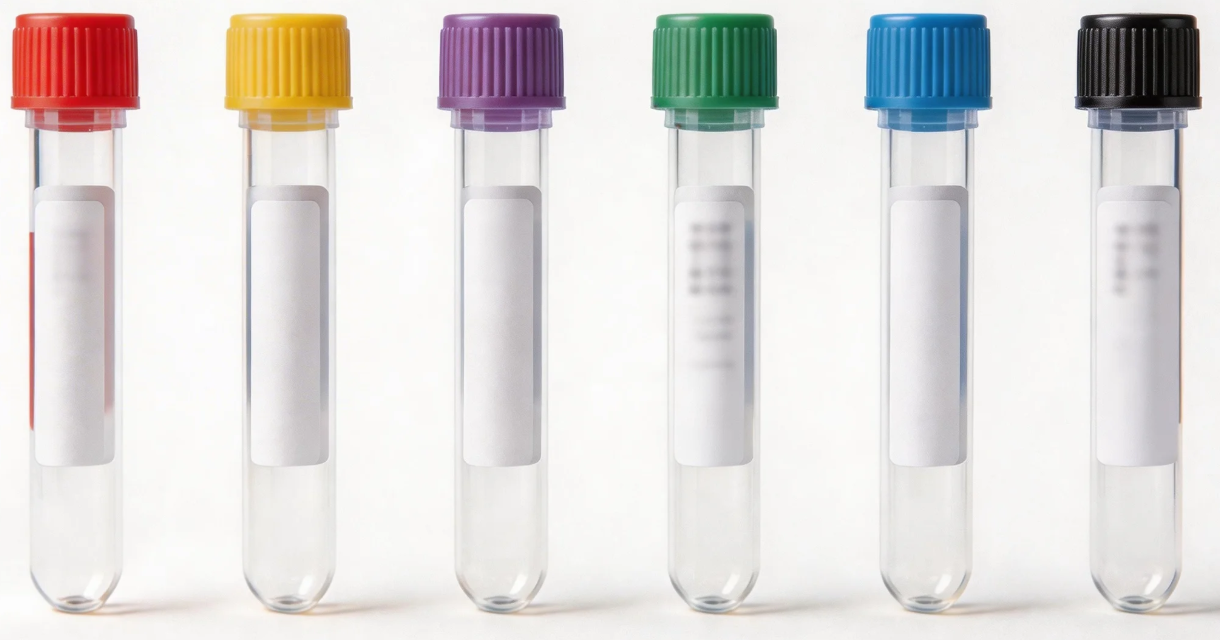
Generally speaking, in ELISA tests, serum samples are recommended to be collected in red, yellow or orange tubes, while plasma samples should be collected in purple or green tubes. Choosing the appropriate collection tubes is a crucial step to ensure the quality of the samples and improve the accuracy and reliability of the ELISA test results.
